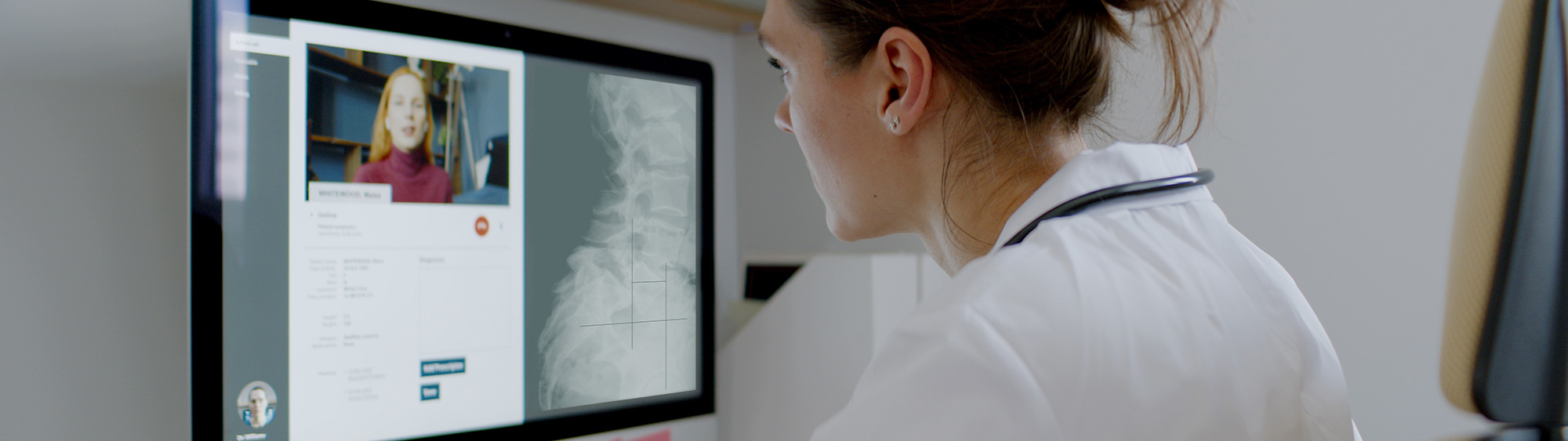
The COVID-19 pandemic has accelerated the adoption of telemedicine around the world, with care for spine patients being no exception. The European Spine Journal recently published “Provider confidence in the telemedicine spine evaluation: results from a global AO Spine study” which provides important context for spine surgeons around the world as they have incorporated telemedicine into their practices. Corresponding author Sravisht Iyer says it highlights some of the limitations of this new platform but also shows some areas where telemedicine might be useful and provides hints towards how we might establish ‘best practices’ as a field moving forward.

The study was a collaborative effort involving 17 authors from 13 institutions in 5 geographic regions: North America, South America, Europe, Africa, and Asia Pacific. An online survey was distributed on May 15, 2020 to AO Spine members worldwide. The survey consisted of 42 questions that were divided into four major themes: global perspectives, challenges and benefits, telemedicine evaluation, and training and research. A total of 485 spine surgeons participated. As Iyer points out, “this study spotlights the crucial leadership role of AO Spine, and the value of an international spine organization in describing and responding to changes in practice patterns around the world.”
“This study spotlights the value of an international spine organization in describing and responding to changes in practice patterns.”
Telemedicine was defined to include video conferencing and phone calls with audio only. The anchor question was “If you or a family member were a patient, do you believe the initial visit can be done through telemedicine?” A total of 74.9% of respondents agreed, while 21.1% were neutral or disagreed. Overall, the majority of respondents felt that telemedicine was at least equivalent to in-person visits for communicative tasks, such as taking a patient history (64.3%), reviewing and explaining imaging (72.3%), and formulating and communicating a treatment plan (67.7%).
In contrast, there was low confidence in telemedicine for the physical-exam-based aspects of patient evaluation, with 94.6% of respondents rating telemedicine as “worse” or “much worse” for assessing neurological deficits, 89.5% giving poor ratings for provocative testing, and 89.0% giving poor ratings for assessing myelopathy.

This dissatisfaction is hardly surprising, but as co-author Dino Samartzis emphasizes, “we engaged the global community with hopes that ‘together’ we can push this field ahead and see it develop properly.” The authors, therefore, identified factors that were significantly associated with increased confidence in using telemedicine to formulate and communicate a treatment plan, and to make an accurate diagnosis.
“Together we can push this field ahead and see it develop properly.”
One factor that was associated with increased confidence was the use of videoconferencing instead of audio-only phone calls. Another factor was whether the provider had performed greater than 50 telemedicine visits at the time of the survey, which was true of 22% of respondents. No reliable differences were found based on region of practice, or specialization in orthopedics compared to neurosurgery. However, those with neurosurgery training expressed increased confidence in telemedicine for imaging review and explanation, compared to their orthopedic-trained colleagues.

Lead author Francis Lovecchio explains that the COVID-19 pandemic has forced providers to recognize the advantages and limitations of telemedicine. “We believe that our survey shows how a dichotomous approach to patient encounters—virtual vs. in-person—vastly underestimates the possibilities of telemedicine.”
“The future of telemedicine lies in its judicious use for certain types of patient encounters,” Lovecchio continues. “For example, video conferencing allows providers to confidently conduct imaging review or pre-surgical discussions, while other evaluations may require in-person visits. As with any new technology, the ultimate test of telemedicine will be whether we can employ the method in a manner that enhances the patient and surgeon experience without compromising our outcomes.”
“The ultimate test will be whether we can employ the method in a manner that enhances the patient and surgeon experience without compromising outcomes.”

Co-author Melvin C. Makhni adds that “everyone recognizes that telemedicine is here to stay, but our study helps build an understanding of global practice patterns, as well as challenges and benefits faced by spine surgeons around the world that will guide the manner in which telemedicine will be optimally integrated into the practice of spine surgery moving forward.”
To move closer towards this goal, a second paper resulting from the same survey explores “Spine surgeon perceptions of the challenges and benefits of telemedicine” and was also published in the European Spine Journal. The study highlights concern about the decreased ability to perform physical exams, possible increased medicolegal exposure, and lack of reimbursement parity compared to traditional visits. Surprisingly, technological issues were not a major concern for physicians, but were reported as a more common challenge for patients. The study also identified regional differences between North America and Africa.
A third paper resulting from this survey explores “Telemedicine in research and training”, also recently published in the European Spine Journal. While a clear majority of survey respondents believe that telemedicine should be incorporated into clinical training, most respondents were not including trainees in telemedicine visits at the time of the survey. The pandemic has upended how the next generation of surgeons is being trained, but this can be turned into an advantage if best practices for patient visits and training protocols can be established.
Samartzis adds that in an age of a pandemic such as this, the telemedicine platform has become increasingly important, but more research is needed. “The strength and novelty of our research initiative via AO Spine is its global nature.”
“Telemedicine is here to stay and AO Spine’s footprint in this area can be transformative.”
“Telemedicine is here to stay and AO Spine’s footprint in this area can be transformative,” Samartzis concludes. “As such, we have started a formal AO Spine Telemedicine Initiative that has brought together worldwide experts in an effort to establish consensus and recommendations for telemedicine in the spine field, cultivate future multicenter research projects, and address policy changes globally—thereby make a lasting impact.” As always, the goal is to provide the best possible care for each patient.
You can find more details of the “Telemedicine & the Spine Surgeon—Spine Surgeon Perspectives and Practices Worldwide” study and all published outcomes here.